- Normal electrical function of the heart
- Sinus node and conducting system disease
- Supraventricular Tachycardia (SVT)
- Atrial Flutter
- Atrial Fibrillation (AF)
- Ventricular Tachycardia (VT)
- Ventricular Fibrillation VF
- Helpful Links
Normal electrical function of the heart
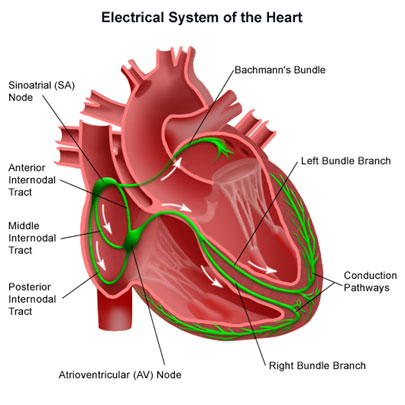
The heart is made up of muscle fibres generating small electrical currents. The co-ordination of these electrical currents results in a wave like action that causes the heart to beat. The electrical wave starts in the sinus or sino-atrial (SA) node in the upper right hand corner of the heart and travels across the two upper chambers, or atria, to a button of tissue – the atrio-ventricular or AV node – and then conducted rapidly to the lower chambers or ventricles via specialised fibres (Purkinje fibres) which are organised into two main bundles – the right and left.
Individual muscle fibres beat at their natural rates – the fastest rate starts in the sinus node which is the heart’s main pacemaker. Its natural rate is about 100 beats/minute and controlled by the (autonomic) nervous system, being slowed by the vagus nerve and, sped up by the sympathetic nerves.
In health, the heart rate is 60 to 100/minute at rest and speeds up with exercise, emotion and rising body temperature. The maximum heart rate depends on age. It is normal for the heart to slow during sleep below these resting values. In the young and athletic people the heart rate is often slower than 60/minute – heart rates may be in the range of 45 to 55/minute at rest.
Heart rhythm disorders can result in heart rates which are too slow (bradycardia) or too fast (tachycardia) and may involve the atria, ventricles, or both.
Sinus node and conducting system disease
If the sinus node does not beat, other heart tissues will usually continue the heart beat but at a slower rate. If these other pacemakers do not cut in, the heart stops until a natural pacemaker does start again. During this pause the heart is not pumping and patients may experience dizziness, a near blackout (pre-syncope) or actually lose consciousness (syncope).

Sinus arrest without an escape rhythm for 2 -3 seconds in a patient with sick sinus syndrome
Commonly, fast and slow heart rates can occur in the same patient such as in the tachy-brady syndrome. Pacemaker tissues usually restart promptly after a period of rapid rhythm but when this tissue is diseased there can be a delay in restarting the heart’s rhythm with symptoms of dizziness or ‘funny turns’. Disease of the AV node and conducting system can delay or reduce the number of electrical impulses reaching the ventricles. This may be obvious on the resting ECG or detected by longer ECG recordings (days to months). The delay shows as delay between the initial or ‘p-wave’ due to electrical activation of the atria and the spike due to the QRS complex when electrical activation of the ventricles occurs.

Heart block in the AV node varies in degree with no conduction at all in 3rd degree block. Unless the ventricles start beating, the heart will stop altogether.
Detecting episodes of heart block allows appropriate treatment to be recommended – either an artificial pacemaker or defibrillator with pacemaker function. The fast heart rhythm, or tachycardia, can then be treated safely without worsening slow heart rhythms.
Supraventricular Tachycardia (SVT)
These arrhythmias are common in otherwise healthy individuals and may be debilitating, because of their unpredictable occurrence and speed during daily life, but are generally not life threatening.

Slow pathway (1) and fast pathway (2). In B an early beat is blocked from conducting via the fast pathway and the normal beat which travelled via the slow pathway now turns back on itself to conduct backwards and then continues in rapid and circular fashion (C).
There are two common types which account for more than 90 % of SVTs. These are AV node junctional reentrant tachycardia (AVJRT) and those due to an accessory or additional electrical connection between the atria and ventricles (Wolff-Parkinson-White syndrome). And there are other, much rarer, types.
The basic mechanism which causes this and many other heart arrhythmias is called ‘re-entry’. After a heart beat occurs there is time when the heart cannot beat again as it is recharging itself (absolute refractory period), then there is a period when a particularly vigorous electrical impulse can initiate a heartbeat (relative refractory period) followed by normal electrical function.
The electrical function of the heart is different in different areas. When there are areas with different electrical function close to each other, the normal even conduction of electrical impulses can be disrupted, especially if a normal beat is followed by an extra beat coming from another area of the heart or ectopic beat. The ectopic beat precipitates re-entry via the slower pathway.

AV node re-entrant tachycardia with re-entry via a slow pathway shown in red.
In AVJRT the re-entry occurs in and around the AV node. Drugs which slow conduction such as beta-blockers or calcium channel blockers can be used to treat it but acutely we give a naturally occurring substance, adenosine, which shows electrical activity throughout the heart briefly stopping the rhythm and allowing normal rhythm to resume. As in all heart arrythmias we can use an external electrical shock to reset the heart’s rhythm (cardioversion) but this is not usually needed in SVT. This arrhythmia is readily cured by an electrical ablation procedure which eliminates the slow pathway and therefore the re-entry circuit.
In normal subjects the only way electrical impulses travel from atria to ventricles is via the AV node but in SVT due to an accessory A-V connection there is an alternative way for electrical impulses to travel from atria to the ventricles. This accessory connection may be obvious on the resting ECG but in other cases is not obvious or ‘concealed’. Conduction can be much more rapid via the accessory pathway than through the AV node (up to 250/min) and this can be dangerous, as atrial fibrillation can lead to ventricular fibrillation when the pathway is able to conduct from atrium to ventricles.

SVT via an accessory pathway on the left lateral side of the left ventricle. During the tachycardia the rhythm travels via the AV node and backwards (retrogradely) to the atria.
Treatment of this is similar to AVJRT but can be more urgent if the patient is compromised. Curing this arrhythmia involves finding the location of the accessory pathways as they may be multiple and then ablating them using high frequency alternating current applied by special catheters under a general anaesthetic or sedation.
Atrial Flutter
Atrial flutter is a type of organised rapid heart rhythm which spins around either of the atria at between 250 to 300 beats/minute and is conducted to the ventricles via the atrioventricular (AV) node. Normally the flutter rate is too fast to conduct to the ventricles and so it is generally conducted in a ratio of between 2:1 and 4:1.
Atrial flutter is caused by the same sorts of causes as atrial fibrillation. Many patients have both and curing atrial flutter can reduce the burden of atrial fibrillation. Treatment of atrial flutter is similar to atrial fibrillation including ant-arrhythmic drugs, electrical cardioversion and ablation procedures. The stroke risk is lower than atrial fibrillation. Curing typical (right atrial) flutter is relatively straightforward with a high success rate (90%) and low complication rate.

Typical ECG of a patient with right atrial flutter shows ‘saw tooth’ waves on the 12 lead ECG.
Atrial Fibrillation (AF)
Atrial fibrillation (AF) is a common heart rhythm disturbance. Instead of a coordinated electrical wave there is chaotic electrical activity with individual or small groups of fibres discharging electrical pulses which do not lead to organised contraction of the atria. The heart rate is much faster than usual and completely irregular.
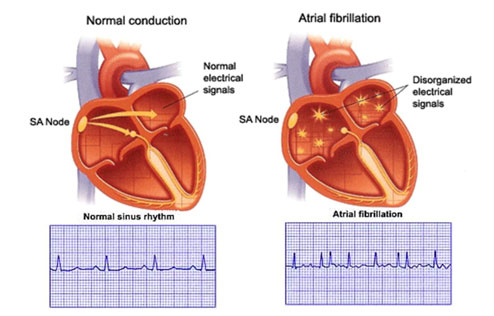
The atria are uneven in shape and have an area on the outer edge – the appendage- where blood flow can stagnate if the atria are not contracting. The blood clot can then leave the heart into the circulation, either during AF or when rhythm and contraction is restored, blocking blood vessels to important organs such as the brain (stroke), kidneys, bowel, or limbs. This is more likely to happen in hearts which have other forms of heart disease such as valve disease or heart failure.
Atrial fibrillation can be triggered by stimulating the vagus (vagal AF) or sympathetic nerves (adrenergic AF). Common vagal triggers include gut disturbances such as drinking cold drinks, nausea, vomiting, indigestion or abdominal pain. Athletes with high vagal nerve activity are prone to it. It is commoner in sleep when the heart rate is slower due to the effect of the vagus nerve on it. Adrenergic triggers include exercise or emotional stress and adrenergic AF is more likely during the day. We commonly see AF triggered by stresses such as infection and major surgery. Sleep apnoea is an increasingly recognised trigger of AF.
Treatment of atrial fibrillation is directed at controlling the rhythm and preventing serious consequences such as worsening heart failure or stroke. Treatments include: drugs, electrical cardioversion and curative procedures.
The two common types of rhythm treatment are intended either to keep the heart in normal rhythm – rhythm control – or slow the heart rate when in atrial fibrillation to a more normal range – rate control. The types of drugs used vary.
There are two types of drugs which lower the risk of stroke: anti-platelet (aspirin, clopidogrel) and anti-coagulant (warfarin or dabigatran) drugs. These drugs can cause bleeding as a side-effect so the type recommended depends on the relative balance of the risks of clotting versus bleeding in individual patients.
Provided there is a low chance of clot inside the heart, we commonly shock the heart back into rhythm (cardioversion) under a short general anaesthetic.

Watchman™ device being placed in the left atrial appendage
Increasingly electrical (electrophysiology) procedures are being used to prevent or cure atrial fibrillation (‘pulmonary vein isolation’ or PVI) when AF causes disabling symptoms. These relatively time consuming procedures may need to be repeated to achieve success. These may also be performed at the time of heart surgery.
Another novel procedure uses a device which is used to reduce the risk of stroke by filling the atrial appendage and avoid the need for anti-coagulant drugs (Watchman™).
Ventricular Tachycardia (VT)
This is a serious heart arrhythmia which can cause sudden death. It affects the ventricles and usually occurs in those with structural heart disease but also occurs in those with genetic conditions affecting the internal chemistry of heart muscle cells (channelopathies including Long QT).
It is usually caused by re-entry (see Supraventricular Tachycardia (SVT)), but in this case it occurs in the border zone between healthy and dead tissue, typically as a result of damage either following a heart attack or heart muscle disease such as cardiomyopathy. It can be treated with drugs but is most effectively treated by either ablation or, more commonly, by implanting an ICD (implanted cardioverter/defibrillator).
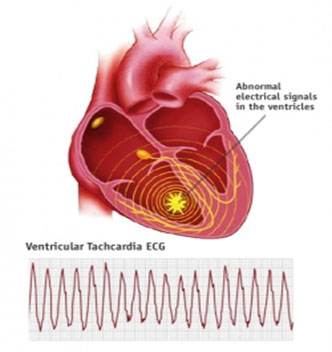
Ventricular tachycardia is a relatively organised arrhythmia and the ventricles do pump to an extent during it. If it is short-lived then it may not affect brain function and therefore consciousness. However, if it is prolonged or ‘sustained’, disturbance of consciousness and sudden death can occur.
Ventricular Fibrillation VF
This is a chaotic and usually fatal arrhythmia. Individual or small groups of ventricular muscle fibres are activated which means no co-ordinated contraction occurs and is rapidly fatal unless the heart is shocked back into normal rhythm promptly.

ECG during ventricular fibrillation (VF)
The main emphasis is on prevention of sudden death in those at high risk (primary prevention) and implanting ICDs in those where an event occurs, is treated and which is likely to recur later (secondary prevention).
